SSM Health Cardinal Glennon Children’s Hospital diabetes care team helps patients live their best lives
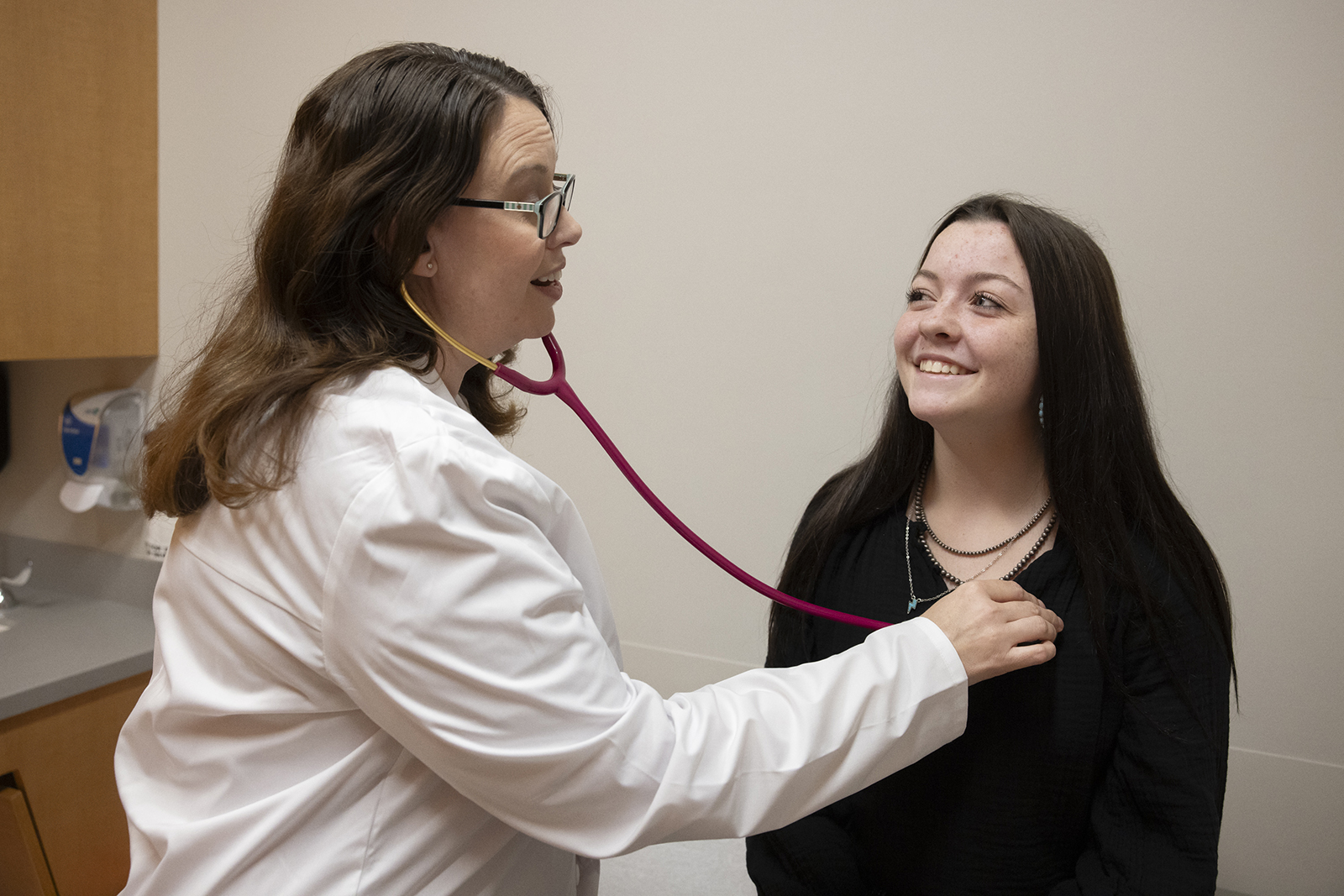
Ezri Landreth was diagnosed with type 1 diabetes when she was 12. Now 16, she takes it in stride.
Sure, she has to be careful that her glucose pump doesn’t come loose when she’s riding horses, and she doesn’t walk around outside barefoot like she used to — wounds don’t heal as easily when you’re diabetic, she explained — but managing the condition has become just another piece of her normal routine.
That’s largely due to the education, support and ongoing care Ezri and her parents, Miranda and Michael Landreth, have received from SSM Health Cardinal Glennon Children’s Hospital, Miranda said. The family makes the hour-and-a-half drive from their home in Jackson to Cardinal Glennon Children’s Hospital’s pediatric specialty services South County location every four months for checkups. In between, they appreciate how accessible the medical team is to answer questions and give instructions over the phone whenever they need it.
“If you’re having an issue, you don’t have to schedule an appointment and wait to come in,” Miranda said. “They walk you through all of it on the phone — new doses, if she’s sick, they walk you through everything. They are just super accessible.”
SSM Health Cardinal Glennon Children’s Hospital pediatric endocrinology team provides diagnosis, treatment and lifestyle management for types 1 and 2 diabetes and other complex endocrine system disorders. Diabetes is a chronic condition that develops when blood sugar levels are too high, which usually happens when the body does not produce enough insulin, does not use insulin effectively, or both.

When a child is diagnosed with diabetes, they’ve often had symptoms like increased thirst, frequent urination or weight loss for several weeks or months before vomiting or other illness brings them to their primary care physician or emergency room, said Dr. Amy Clark, a pediatric endocrinologist and diabetes program director at SSM Health Cardinal Glennon Children’s Hospital.
About three-quarters of their pediatric diabetes patients have type 1 diabetes, but they have seen an increase in type 2 diabetes in correlation with the rise of childhood obesity, Dr. Clark said.
Once diagnosed, the child and family stay at the hospital for about two days of education and monitoring. They learn how to give insulin shots, check blood sugar levels, count carbohydrates in food and adjust dosages accordingly.
“It’s pretty life-changing. It’s a lot of shots. It’s a lot of change in your routine,” Dr. Clark said. “But our team is very good about teaching everyone the skills, making everyone comfortable, and by and large, most of our patients are back in school usually the day following going home.”

Once the family is back home, nurse navigator Alex McCracken and other members of the medical team check in frequently to see how they are navigating their new normal. Parents are sometimes afraid their children won’t be able to participate in their regular activities or eat birthday cake, but with the right knowledge, children can continue to participate in all the same things, he said. The child psychology team also follows up with newly diagnosed families in the first month to offer support.
Dr. Clark — a type 1 diabetic herself — has seen diabetes treatment evolve over the years. One of the biggest technological leaps was the continuous glucose monitor, which checks blood sugar every five minutes and takes away the need for multiple finger sticks a day. Insulin pumps, which continuously provide insulin to the body, have also grown in popularity. In the past 10 years, insulin pumps have been integrated with continuous glucose monitors and can adjust insulin dosage based on current blood sugar readings.
“Patients still have to carb count and enter what they’re eating in their insulin pump, but if they maybe underestimate the amount of carbs or overestimate, on the back end, the pump can see where their blood sugar is going, and if it’s going up, give more insulin,” she said.
Newly diagnosed patients always start with insulin shots and finger sticks, though, because if a glucose monitor or insulin pump malfunctions, they need to be able to continue dosing and monitoring while waiting for it to be fixed, Alex said.
As pediatric specialists, one of their goals is to prepare teenagers to take more ownership of their medical care as they prepare to transition to adulthood. Doctors and nurses work with patients on age-appropriate skills, building up toward independence over the years.
“When they get to driving age, we really want them to be able to do the skills themselves,” Alex said. “We want to get our kids as much independence as we can, especially into those late teenage years.”
The team also offers a quarterly care for caregivers class, where siblings, grandparents, aunts and uncles, teachers or other adults in the child’s life can come learn about diabetes care.
It’s all part of living out the SSM Health mission: “Through our exceptional health care services, we reveal the healing presence of God.”
“We try to provide compassionate, comprehensive care for all our patients, and just try to help them live their best life. Usually when parents ask about things like sports — can they do this, can they do that? I’m like, we can help you. You can do anything you want,” Dr. Clark said. “We’re not going to let diabetes rule your life. We’re going to run your diabetes well so that you can do whatever you want with your life. We’re just here to help you with that.”